Key Takeaways
- DR upgrades deliver 96% productivity increases and 71% patient wait time reductions by eliminating processing delays, enabling instant image QC, and automating PACS routing.
- Modern DR panels achieve 67-75% DQE compared to 30% for CR systems, enabling 43-67% radiation dose reductions while improving diagnostic image quality through superior contrast, resolution, and noise performance.
- Integration discipline prevents the 84% IT project failure rate through DICOM-compliant worklist connectivity, auto-routing rules, and documented downtime workflows.
- Baseline measurement and target-setting before installation enable objective ROI proof through tracked KPIs with the first 90-day optimization driving sustained improvements.
- Standardized protocols and continuous training determine whether technology investment delivers results; consistent technique charts and QC thresholds prevent “new tech, old habits” failures.
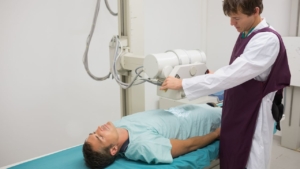
Digital radiography (DR) upgrades replace film or computed radiography (CR) systems with flat-panel detectors that deliver images instantly. The change eliminates physical cassette handling, chemical processing, and manual image routing, steps that add minutes to every exam and create bottlenecks across departments. Evidence shows DR integration drives 96% productivity gains and cuts patient wait times by 71%, transforming both operational efficiency and care delivery.
This comprehensive guide examines the quantifiable benefits, implementation pitfalls, and best practices for DR upgrades based on peer-reviewed research and real-world case studies.
What Is A Digital Radiography Upgrade, And What Changes In Day-To-Day Imaging Operations?
A DR panel upgrade swaps analog or CR cassettes for digital flat-panel detectors (wired or wireless) that send images directly to PACS within seconds. Day-to-day operations shift from physical plate transport and processing queues to instant image review, immediate retakes, and automated routing to radiologists.
CR vs DR Workflow Differences
| Workflow Step | CR Method | DR Method | Typical Delay Removed |
| Room-based exams | Cassette to reader → processing queue | Image appears instantly | 3–8 minutes |
| Portable exams | Transport cassette to reader | Wireless panel sends immediately | 5–15 minutes |
| Image availability | After processing + manual routing | Auto-routed to PACS instantly | 10–30 minutes |
| Repeat handling | Re-expose → transport → re-process | Retake within seconds | 5–10 minutes |
What typically changes in a DR upgrade:
- Detectors: Wired/wireless flat panels; automatic exposure detection (AED)
- Software: Real-time processing, integrated worklists, QC tools, exposure index monitoring
- Integration: RIS/PACS/EMR auto-routing via DICOM modality worklist (MWL)
- QA/QC: Exposure index (EI) tracking replaces film density checks; automated reject tracking
Why Do Departments Upgrade To DR When The Goal Is Better Workflow And Patient Care?
DR upgrades target operational bottlenecks that slow imaging workflows and delay clinical decisions. The 71% reduction in patient wait times (43.5 hours to 4.62 hours) and 11% patient satisfaction stem from eliminating processing delays and automating image routing. These DR system benefits extend beyond equipment performance to fundamentally reshape patient care enhancement.
Workflow constraints DR commonly fixes:
- ED: Surge capacity limits, slow triage imaging, delayed stat reads, transport bottlenecks
- Inpatient: Low portable throughput, isolation protocol delays, after-hours staffing gaps
- Outpatient: Schedule compression, late-start cascades, poor room utilization
- Ortho/trauma: High repeat rates from delayed feedback, time-critical surgical planning
Patient-care improvements:
- Less time in painful positions; fewer repositions
- Fewer repeat exams and callbacks
- Shorter waits and clearer expectations
- Faster clinical decisions (admit/discharge/OR planning)
How Does A DR Upgrade Improve Workflow Speed And Throughput In Real Imaging Scenarios?
DR removes delays from image processing (45% reduction documented) and task execution (40% efficiency improvement), compressing exam cycle times and increasing daily capacity without adding staff or rooms. Modern digital radiography equipment continues to accelerate workflows through intelligent automation.
Where DR removes steps:
- Eliminates cassette handling and transport
- No reader queues or processing failures
- Auto-send to PACS eliminates manual routing
- Instant image review replaces delayed QC
Room turnaround improvements:
- Faster QC and immediate retake decisions before the patient leaves the table
- Reduced “image missing” troubleshooting from automated routing
- Predictable 2–3 minute cycle times enable tighter appointment slots
Portable imaging throughput changes:
- Wireless panels eliminate cassette runs to the central reader
- Faster isolation-room workflows avoid contamination protocols
- Improved bedside QC reduces repeat trips
- Auto-routing with barcode matching eliminates wrong-patient errors
How Does DR Reduce Repeats, Rejects, And Rework That Slow Teams Down?
DR’s instant image feedback enables technologists to catch errors before patients leave the room, eliminating the “develop and hope” cycle. Immediate quality checks, exposure index monitoring, and side-by-side comparison tools cut repeat exams by catching positioning errors, technique inconsistencies, and artifacts in real time.
Common reject/repeat drivers:
- Positioning errors: Rotation, insufficient angulation, improper landmarks
- Anatomy cutoff: Incomplete joint visualization, missing fracture segments
- Motion: Unsharp anatomy from patient movement
- Artifacts: Grid cutoff, radiopaque objects, detector dust/damage
- Exposure inconsistency: Over/underexposure, inconsistent EI values across technologists
Reject analysis for action: Track patterns across technologists, shifts, rooms, and exam types to identify systemic issues. Trends reveal training gaps, equipment problems, and workflow breakdowns, enabling targeted fixes.
Actions by pattern:
- High rejects by technologist → positioning coaching, anatomy refresher
- High rejects by exam type → protocol review, technique chart updates
- High rejects by room/detector → equipment calibration, grid alignment verification
- Artifact patterns → detector cleaning/replacement, handling retraining
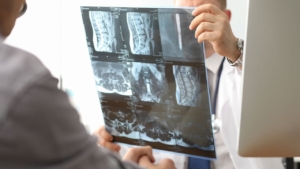
How Does A DR Upgrade Improve Image Quality And Diagnostic Confidence?
Modern DR panels deliver 67-70% DQE compared to 30% for CR systems, a 100% quantum efficiency improvement that produces sharper, lower-noise images at equivalent or reduced radiation doses. AI-enhanced DR systems achieve 83% diagnostic accuracy and 81% sensitivity, further supporting clinical decision-making.
Superior detector performance (higher DQE, smaller pixels, wider dynamic range), standardized processing algorithms, and immediate QC feedback combine to accelerate patient throughput while improving diagnostic yield.
Exam types where quality gains are most noticeable:
- Portable chest: Clearer lung parenchyma despite difficult positioning
- Ortho extremities: Sharper trabecular detail for subtle fracture detection
- Abdomen: Enhanced bowel gas pattern distinction, reduced scatter artifacts
- Trauma views: Superior bone-soft tissue contrast in challenging projections
- Larger patients: Wider dynamic range maintains quality across varying tissue densities
How Can DR Support Dose Optimization While Keeping Images Diagnostically Useful?
DR’s superior DQE enables dose reductions of 43-67% while maintaining or improving diagnostic quality, documented across shoulder imaging (43% lower), hip RSA studies (64% lower), and interventional cardiology (56-67% lower patient dose). Occupational dose also drops 33%, protecting staff during high-volume procedures.
Exposure Index (EI) Workflow Use
| Concept | What It Indicates | What “Out of Range” Suggests | Recommended Response |
| Underexposure pattern | EI below target range | Technique chart too conservative, AED malfunction | Review technique factors, test AED calibration |
| Overexposure pattern | EI above target range | “Dose creep” from over-cautious technique | Adjust technique charts downward; emphasize ALARA |
| Outlier by technologist | Techs consistently outside targets | Training gap, fear of underdosing | Individual coaching, technique chart re-education |
| Outlier by room/detector | Specific equipment produces high/low EI | Calibration drift, detector sensitivity variation | Schedule calibration, test uniformity, replace aging equipment |
Practical ways to prevent dose creep:
- Set exposure targets by exam type and body habitus
- Use EI/DI feedback routinely, not only in audits
- Audit repeats + exposures together
- Reinforce collimation/positioning to avoid “dose to fix blur”
- Update technique charts after 30-90 day go-live learnings
How Does A DR Upgrade Improve Patient Experience And Patient-Centered Care?
DR upgrades deliver a 71% reduction in patient wait times (43.5 hours to 4.62 hours median) and drive 11% increases in patient satisfaction. Instant image review lets technologists confirm quality before releasing patients from painful positions, no waiting for cassette processing to discover positioning errors. Fewer repeats mean less radiation exposure, less time on hard tables, and fewer repositioning demands.
Repeats signal incompetence to patients, eroding confidence and increasing anxiety. Standardized DR workflows with immediate feedback eliminate most “we need to start over” moments, demonstrating professionalism and building trust.
Ways predictable workflows improve communication:
- Clearer ETA for results (consistent 2-3 minute time-to-image)
- Fewer missing images or misrouted studies
- Better coordination for transport/bedside imaging
- More consistent patient instructions and expectations
What Interoperability And Documentation Benefits Come With Modern DR Workflows?
Modern DR panels integrate seamlessly with PACS through DICOM compliance, enabling automatic worklist population, demographic accuracy, and intelligent routing rules that eliminate manual data entry and reduce wrong-patient errors. DICOM modality worklist (MWL) pulls patient demographics and exam orders directly from RIS, auto-populates acquisition console fields, and routes completed studies to correct PACS destinations, multiplying the time savings from faster DR capture.
Integration benefits:
- Patient info pre-loaded from RIS; no manual typing
- Eliminates transcription errors and duplicate medical record numbers
- Studies flow to correct radiologist worklists without manual sorting
- Barcode/RFID verification prevents mislabeled portables
- Real-time dashboards show exam status; managers identify slowdowns immediately
What Operational And Financial Benefits Should You Quantify When Justifying A DR Upgrade?
DR upgrades deliver 96% productivity increases and 791% five-year ROI when integrated with advanced workflows. The 45% reduction in image processing time and 40% workflow efficiency improvement translate directly to increased exam capacity, reduced overtime costs, and faster revenue cycle completion.
Cost drivers that improve after DR:
- Fewer repeats reduce wasted exposures and technologist time
- Higher exams-per-hour rate reduces backlog-driven overtime
- Fewer moving parts means less maintenance downtime
- Eliminate reader maintenance contracts and plate replacement cycles
- Predictable cycle times prevent schedule overruns
ROI Productivity Measures
| KPI | Calculation | Data Source | Target |
| Studies/hour | Total exams ÷ total room hours | RIS, scheduling system | 15-30% increase |
| Room utilization % | (Actual exam time ÷ scheduled time) × 100 | Scheduling logs | 75-85% |
| Time-to-image | PACS timestamp – exposure timestamp | PACS logs | <30 seconds |
| Exam cycle time | Exit timestamp – entry timestamp | Manual observation | 20-40% reduction |
| Portable exams/shift | Portable count ÷ portable tech shifts | RIS, staffing records | 30-50% increase |
How Do You Plan, Implement, And Validate A DR Upgrade So Benefits Show Up In Your Metrics?
Successful DR upgrades require baseline measurement, clear targets, structured testing, and post-go-live optimization. Vieworks’ DICOM-compliant, retrofit-friendly design and AI-enhanced diagnostic tools (VXCAD-CXR) demonstrate that modern DR systems integrate seamlessly when implementation follows disciplined planning.
Retrofit vs Full Room Replacement Decision Factors
| Factor | Retrofit Best When | Replacement Best When |
| Room condition | Equipment <7 years old and functional | Equipment >10 years, frequent repairs |
| Volume | Moderate volume; room meets most needs | High volume; need advanced features |
| Portability needs | Need wireless for portables + fixed room | Primarily fixed-room work |
| Service support | Vendor supports detector integration | OEM ending support, parts unavailable |
Integration and routing planning checklist:
- Worklist configuration and patient matching rules
- Destination routing rules by exam type/location/priority
- QC checkpoints and exception handling
- Downtime workflow and failover plan
- Test cases for common/edge scenarios
Training + standardization plan:
- Technique charts by exam type/body habitus
- Positioning/collimation refresh tied to top reject reasons
- QC decision rules (when to retake vs adjust processing)
- Portable workflow playbook
- Competency checks during go-live week and 30-day follow-up
Go-Live Optimization Plan
| Timeframe | Focus Area | Expected Change | Corrective Actions |
| Week 1 | System uptime, basic workflow | Initial learning curve | 24/7 vendor support, daily huddles |
| Weeks 2-4 | EI/DI consistency, technique refinement | 10-20% reject rate improvement | Adjust technique charts, retrain on outliers |
| Month 2 | Reject/dose consistency | Reject rate <5%, EI compliance >85% | Individual coaching, protocol updates |
| Month 3 | Productivity + patient flow | 20-30% productivity gain | Schedule optimization, eliminate bottlenecks |
What Pitfalls Can Prevent A Dr Upgrade From Delivering Workflow And Patient-Care Improvements?
Healthcare IT integration projects fail 84% of the time; success depends on standardization, training, and integration discipline, not just equipment quality. New detector technology paired with old habits produces disappointing results.
Fixes that reduce repeats:
- Protocol alignment: Standardize positioning guides and technique charts across all shifts
- Individual feedback on reject patterns with side-by-side image review
- Weekly team reviews of top reject reasons
- Formal training on detector handling and charging
- Clear pass/fail criteria that all technologists apply identically
Integration gaps that create hidden delays:
- Auto-routing rules are incomplete or disabled; manual destination selection
- RIS-PACS interface gaps force manual order entry
- ED stat studies are routed to the general queue instead of the dedicated stat worklist
- No documented downtime procedure for local storage and batch-send recovery
- No dashboard showing studies in progress for X minutes or failed sends
Which KPIs Should You Track After Go-Live To Prove Improved Workflow And Patient Care?
Target benchmarks from research, 71% wait time reduction, 96% productivity increase, 45% processing time reduction, 56-67% dose reduction, and provide concrete goals for measuring DR upgrade success.
Key Workflow KPIs:
- Time-to-image: <30 seconds (vs. 3-8 min CR baseline)
- Exam cycle time: 20-40% reduction from baseline
- Portable throughput: 30-50% increase from baseline
- Backlog/queue time: <5% of daily volume
Quality KPIs:
- Reject rate: <5% overall; >7% for 2 weeks triggers action
- EI/DI compliance: >90% within institutional target range
- Callback indicators: <2% of exams
Patient-Care KPIs:
- Patient wait time: 30-50% reduction (benchmark: 71% achievable)
- ED imaging-to-decision: Reduce delays by 20-30%
- Satisfaction signals: Track imaging-specific comments from HCAHPS
What Common DR Upgrade Questions Should You Answer For Stakeholders?
Phasing an upgrade without disrupting throughput: Staged implementations minimize risk by upgrading one room at a time. Start with a moderate-volume room to test workflows, then roll out to the remaining fixed rooms before tackling portables. Schedule installations during low-volume periods, plan 1-3 days of downtime per room with clear diversion protocols.
Detector Features That Most Affect Workflow
| Feature | Why It Matters | Questions to Ask Vendors |
| Wireless | Eliminates cables; faster portable positioning | Battery life per charge cycle? Swap protocol? |
| Battery life | Determines exams per charge, swap frequency | How many exams on full charge? Replacement cost? |
| Durability | Survives drops, impacts, transport | Drop-test ratings? Repair vs. replace criteria? |
| AED reliability | Consistent exposure detection | AED failure rate? Calibration schedule? |
| Infection control | Cleaning between patients, isolation protocols | Approved cleaning agents? Wipe-down durability? |
Research Note: Vieworks VIVIX wireless cesium panels feature an award-winning design (iF Design Award 2018, Red Dot Award 2018), demonstrating industry recognition for combining advanced detector technology with ergonomic design.
Ensuring faster clinical decisions: Auto-routing rules must send ED stat studies to dedicated high-priority worklists with push notifications to on-call radiologists. Consistent study labeling helps radiologists triage efficiently. Fewer missing studies from reliable integration eliminates “where’s my image?” phone calls. Tighter closed-loop communication confirms when critical findings reach ordering physicians.
What Are the Next Steps If You’re Considering A DR Upgrade?
“This week” project scoping actions:
- Confirm stakeholders (imaging, IT, radiology, nursing/ED, biomed, finance)
- Pull 60-90 days baseline data (workflow, quality, dose, wait times)
- Define 5-8 success metrics with achievable targets
- Map current pain points to specific DR equipment solutions
- Draft phased approach and downtime plan
What to request from vendors:
- Workflow demo scenarios (ED surge, portable isolation, stat routing)
- Reporting/analytics capabilities (reject tracking, EI/DI monitoring, throughput)
- Integration plan and DICOM conformance statements
- Training plan with competency validation approach
- Service SLAs, uptime expectations, replacement logistics
DR upgrades deliver measurable improvements in workflow speed, image quality, radiation dose optimization using proper contrast, and patient satisfaction, but only when implementation combines technology investment with process standardization, integration discipline, and continuous optimization.
Ready to explore how DR technology can transform your imaging workflows? Contact Spectrum X-Ray’s sales team to discuss your facility’s specific needs and schedule a customized workflow assessment.