Healthcare facilities face critical equipment decisions that directly impact diagnostic capabilities and operational efficiency. Selecting between ultrasound and X-ray technology requires evaluating clinical applications, safety profiles, cost structures, and workflow integration. Both modalities serve distinct diagnostic purposes, and understanding their fundamental differences ensures facilities invest in equipment aligned with patient demographics and service offerings.
The choice between these imaging technologies extends beyond initial purchase price to encompass maintenance requirements, operator training, and long-term return on investment. Facilities must balance clinical versatility against equipment specialization while considering patient throughput and diagnostic accuracy. This analysis examines technical specifications, cost comparisons, and strategic considerations to guide purchasing decisions.
Key Takeaways
- Ultrasound machines use sound waves and emit no radiation, while X-ray systems use ionizing radiation for skeletal imaging
- Ultrasound equipment costs $3,000-$120,000 compared to X-ray systems at $45,000-$200,000
- Ultrasound excels at soft tissue visualization, but cannot penetrate bone effectively
- X-ray imaging provides superior skeletal detail but offers limited soft tissue contrast
- Cost factors account for 28% of purchasing decisions, while performance weighs 24%
What Are Ultrasound and X-Ray Machines?
Ultrasound and X-ray machines represent foundational diagnostic imaging technologies with distinct operational principles. Each modality uses different physics to generate images, resulting in unique clinical applications and safety profiles.
How Does Ultrasound Imaging Work?
An ultrasound machine generates high-frequency sound waves that penetrate tissue and create real-time dynamic images of internal structures. The transducer probe both emits acoustic waves and receives reflected echoes, which computer processing converts into visual representations. This technology enables continuous visualization of moving structures like beating hearts and developing fetuses without exposing patients to ionizing radiation.
The sound wave frequency determines imaging depth and resolution characteristics. Higher frequencies produce superior image detail but cannot penetrate deeply, while lower frequencies reach deeper structures with reduced resolution.
How Do X-Ray Systems Create Images?
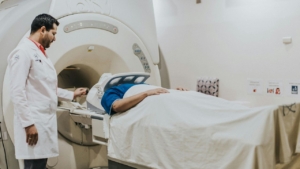
Digital X-ray systems offer lower radiation doses and immediate image display without chemical processing. Modern detectors convert X-ray photons directly into digital signals, eliminating film development time and enabling instant image enhancement through software manipulation. Analog X-ray represents the traditional film-based approach requiring chemical processing, though most facilities have transitioned to digital platforms for improved efficiency and reduced radiation exposure.
X-ray technology relies on electromagnetic radiation passing through the body to create two-dimensional projection images. Dense tissues like bone absorb more radiation and appear white, while soft tissues allow greater transmission and appear darker.
What Are the Key Clinical Uses of Each Modality?
Ultrasound proves excellent for cardiovascular assessment, obstetric monitoring, and abdominal organ evaluation. Real-time imaging capabilities make ultrasound ideal for guiding needle biopsies and monitoring fetal development throughout pregnancy. The technology also serves point-of-care applications in emergency departments where immediate soft tissue assessment guides treatment decisions.
X-ray imaging excels at identifying bone fractures and evaluating chest pathology, including pneumonia and cardiac enlargement. The modality provides rapid skeletal assessment essential in trauma situations and orthopedic evaluations.
What Are the Main Differences Between Ultrasound and X-Ray Machines?
Fundamental technological differences between ultrasound and X-ray create distinct advantages and limitations for each modality. Understanding these contrasts enables facilities to match equipment capabilities with clinical requirements and patient safety priorities.
How Do Ultrasound and X-Ray Compare on Safety and Radiation Exposure?
Ultrasound uses acoustic waves that produce no ionizing radiation, making it completely safe for repeated examinations and vulnerable populations. Pregnant women undergo multiple ultrasound scans throughout pregnancy without radiation risk to the developing fetus. This safety profile has driven widespread adoption of portable ultrasound units across emergency departments and intensive care units where frequent monitoring occurs.
X-ray systems expose patients to ionizing radiation that carries cumulative health risks with repeated exposure. Digital X-ray technology has reduced radiation doses by 50-80% compared to analog film systems, but radiation safety protocols remain essential. Facilities must balance diagnostic benefit against radiation exposure, particularly for pediatric patients and pregnant women.
What Are the Differences in Image Quality and Diagnostic Capabilities?
Ultrasound quality remains highly operator-dependent, requiring skilled technologists to position probes correctly and recognize anatomical landmarks. Image interpretation demands significant training because ultrasound produces grayscale images where tissue differentiation relies on subtle echogenicity variations. Ultrasound suffers from limited penetration through bone and air-filled structures, preventing visualization of brain tissue through an intact skull or lung parenchyma.
X-ray systems generate images limited to two-dimensional projections that compress three-dimensional anatomy onto flat planes. Overlapping structures can obscure details when multiple tissues align in the X-ray beam path, potentially hiding small fractures or lung nodules. X-ray demonstrates poor soft tissue visualization because muscle, fat, and organs display similar radiographic density, appearing as uniform gray zones.
How Does Portability and Operator Dependency Vary?
Portable ultrasound devices range from handheld units weighing under two pounds to cart-based systems offering advanced imaging modes. This portability enables bedside examinations in intensive care units and emergency departments, where the benefits of portable X-ray systems include eliminating patient transport risks for critically ill individuals. Ultrasound requires minimal setup time, allowing clinicians to obtain images within seconds of patient contact.
X-ray equipment traditionally requires dedicated rooms with radiation shielding and fixed mounting systems. Portable X-ray units exist for bedside imaging but remain substantially larger and heavier than ultrasound alternatives, typically requiring two staff members for safe positioning.
When Should You Choose Ultrasound Over X-Ray?
Clinical scenarios involving soft tissue evaluation, real-time imaging needs, and radiation-sensitive populations favor ultrasound as the primary diagnostic imaging tool. Facilities serving obstetric patients or requiring frequent cardiovascular assessments benefit from investing in advanced ultrasound capabilities.
Which Conditions Best Suit Ultrasound Imaging?
Ultrasound serves as the gold standard for obstetric care throughout all pregnancy trimesters. Cardiovascular applications include echocardiography for heart valve assessment, venous thrombosis detection, and vascular access guidance during central line placement. Abdominal ultrasound effectively evaluates gallbladder disease, kidney stones, liver pathology, and appendicitis in pediatric patients.
Musculoskeletal ultrasound identifies tendon tears, joint effusions, and soft tissue masses with dynamic assessment capabilities. Emergency medicine physicians use focused assessment with sonography for trauma (FAST) examinations to detect internal bleeding in unstable patients.
How Does Patient Demographics Influence the Choice?
Spending on imaging remains consistently higher for females than males between ages 14-70, driven largely by obstetric and gynecologic ultrasound utilization. Facilities serving reproductive-age women require robust ultrasound capabilities to meet patient demand and maximize reimbursement opportunities. Peak imaging spending occurs between ages 80-85 at $1,415-$1,559 per person annually, reflecting increased diagnostic needs in geriatric populations.
Imaging represents the largest share of healthcare spending at age 38 for men (9.0%) and age 44 for women (12.4%). These demographic patterns should inform equipment purchasing decisions based on specific patient population characteristics.
What Are the Limitations of Ultrasound That Affect Decision-Making?
Ultrasound provides a smaller field of view compared to X-ray, requiring multiple probe positions to survey large anatomical regions. Examinations of obese patients present technical challenges because increased tissue depth degrades image quality and limits visualization of deep structures. Ultrasound cannot image deep structures effectively when sound waves must traverse more than 15-20 centimeters of tissue, making it unsuitable for certain abdominal applications in large patients.
Bone cortex reflects virtually all ultrasound waves, preventing evaluation of brain tissue, spinal cord, and bone marrow. Gas-filled structures, including lungs and bowel, create artifacts that obscure adjacent anatomy, limiting ultrasound’s utility in chest imaging and gastrointestinal evaluation.
When Is X-Ray the Preferred Imaging Modality?
Skeletal trauma, chest pathology, and rapid throughput requirements make X-ray the preferred initial diagnostic imaging approach. Emergency departments rely on X-rays for immediate assessment of fractures, dislocations, and life-threatening chest conditions requiring prompt intervention.
Which Clinical Scenarios Demand X-Ray Imaging?
Bone fractures require X-ray evaluation to determine fracture pattern, alignment, and treatment planning for orthopedic intervention. Chest X-rays rapidly identify pneumonia, pneumothorax, pulmonary edema, and cardiac enlargement in acutely ill patients presenting with respiratory symptoms. Dental practices depend on X-ray systems for caries detection, periodontal assessment, and pre-extraction evaluation of tooth root anatomy.
Joint dislocations and foreign body localization benefit from X-rays’ superior spatial resolution and bone contrast. Abdominal X-rays detect bowel obstruction and pneumoperitoneum, indicating visceral perforation, though ultrasound and CT have largely replaced X-ray for detailed abdominal evaluation.
How Do Digital and Analog X-Ray Systems Differ in Use?
Digital X-ray technology enables immediate image display without chemical processing, reducing patient wait times from 10-15 minutes to under 30 seconds. Software enhancement capabilities allow radiologists to adjust contrast, magnify regions of interest, and measure anatomical structures without repeat exposures. Facilities considering upgrades should evaluate how to choose the right DR system based on patient volume and workflow requirements.
Analog X-ray systems require ongoing film and chemical supply costs that digital systems eliminate through reusable detectors. Digital integration with picture archiving and communication systems (PACS) enables instant image distribution to referring physicians and remote radiologists.
What Constraints Affect X-Ray Utility in Certain Settings?
X-ray systems require substantial infrastructure, including radiation shielding, electrical capacity, and regulatory compliance with state radiation safety programs. Installation costs can exceed equipment purchase price when facilities lack existing radiographic suites and must construct lead-lined walls meeting regulatory specifications. Mobile practices and rural clinics face logistical challenges in transporting and operating X-ray equipment compared to portable ultrasound alternatives.
Radiation exposure limits repeat imaging frequency, particularly in pediatric populations, where lifetime cancer risk from cumulative radiation remains a concern. Pregnant patients require alternative imaging modalities during early gestation when fetal radiosensitivity peaks.
How Do Costs and Maintenance Influence Equipment Selection?
Total cost of ownership extends beyond the initial purchase price to encompass installation, maintenance, supplies, and equipment depreciation over the operational lifespan. Financial planning must account for ongoing service agreements, replacement parts, and potential revenue generation through reimbursement rates.
What Are the Price Ranges for Ultrasound Vs. X-Ray Machines?
Budget ultrasound systems cost $3,000-$7,000 while comparable X-ray equipment ranges from $45,000-$75,000 for basic units. Mid-range ultrasound machines priced at $15,000-$25,000 offer advanced imaging modes compared to X-ray systems costing $75,000-$150,000 with digital detector technology. Premium ultrasound platforms reach $50,000-$120,000 while high-end X-ray systems cost $150,000-$200,000 for advanced applications.
Per-examination costs demonstrate ultrasound’s economic efficiency at $200-$500 per scan versus X-ray at $100-$300 per study. Facilities must evaluate cost comparison factors, including reimbursement rates, patient volume projections, and competitive positioning within local healthcare markets.
How Do Maintenance and Service Requirements Compare?
Ultrasound machines require minimal routine maintenance beyond transducer cable inspection and software updates performed during annual preventive maintenance visits. Probe replacement represents the primary long-term cost, with transducers costing $3,000-$15,000 depending on imaging frequency and specialized applications. Facilities should establish protocols for regular ultrasound machine maintenance to maximize equipment lifespan and imaging performance.
X-ray systems demand more intensive service, including tube replacement every 3-7 years at costs ranging from $15,000-$40,000 for digital systems. Detector panel failures represent a significant expense, with replacement costs exceeding $60,000 for flat-panel digital detectors requiring specialized calibration.
What Business Models Can Reduce Financial Burden?
Refurbished equipment offers the same-as-new performance at 40-60% lower acquisition costs for facilities managing capital constraints. Reimbursable trade-in programs allow facilities to upgrade technology while recovering residual value from existing equipment, reducing net investment requirements. Pay-per-scan arrangements shift financial risk from facilities to equipment vendors, eliminating upfront capital expenditure in exchange for per-examination fees.
Independent service organizations provide maintenance at 20-40% lower annual costs compared to original equipment manufacturer contracts. Facilities must balance cost savings against response time guarantees and parts availability when selecting service providers.
How Do Consumer Preferences and Accessibility Impact Modality Adoption?
Geographic location, demographic characteristics, and facility resources create disparities in imaging access that influence equipment selection priorities. Understanding utilization patterns enables facilities to align equipment capabilities with actual patient demand rather than theoretical clinical applications.
How Do Age and Gender Affect Imaging Utilization?
Peak imaging spending occurs between ages 80-85 at $1,415-$1,559 per person annually, reflecting increased diagnostic needs for cardiovascular disease, cancer screening, and musculoskeletal conditions. Facilities serving geriatric populations benefit from investing in both modalities to address diverse pathologies across organ systems. Imaging represents the largest share of healthcare spending at age 38 for men (9.0%) and age 44 for women (12.4%), highlighting the importance of diagnostic imaging capabilities for middle-aged populations.
Gender differences in utilization patterns stem from obstetric ultrasound, breast imaging, and gynecologic applications, driving higher female spending. Male patients demonstrate greater X-ray utilization for traumatic injuries and occupational health screening examinations.
What Are the Urban Vs. Rural Disparities in Access?
Only 22.2% of rural patients live within a 30-minute drive of specialized screening centers compared to 83.2% of urban patients with convenient access. Rural areas face significant infrastructure gaps with fewer advanced imaging facilities, creating opportunities for mobile services and point-of-care ultrasound programs. Transportation barriers and limited specialist availability make portable ultrasound particularly valuable in underserved regions where patients cannot easily travel for diagnostic services.
Urban facilities face greater competition, requiring differentiation through advanced technology and rapid turnaround times. Higher patient volumes in metropolitan areas support investment in premium equipment with enhanced throughput capabilities.
How Does Patient Comfort Factor into Modality Choice?
Patient comfort accounts for 4% of purchasing decisions, though this metric significantly influences patient satisfaction scores and facility reputation. Ultrasound examinations involve minimal discomfort beyond gel application and probe pressure, making them preferable for anxious patients and pediatric populations. X-ray positioning requirements can cause pain in trauma patients with acute injuries requiring uncomfortable anatomical alignment for diagnostic views.
Examination duration influences patient experience, with X-ray imaging completed in 5-10 minutes compared to ultrasound studies requiring 20-45 minutes, depending on complexity. Facilities prioritizing patient experience should consider the importance of high-quality imaging equipment that balances diagnostic capability with examination efficiency.
What Performance Metrics Should Guide Your Purchasing Decision?
Objective evaluation criteria enable facilities to compare competing systems and vendors using standardized benchmarks aligned with operational priorities. Weighting decision factors according to facility-specific needs ensures equipment selection supports strategic objectives rather than defaulting to the lowest initial cost.
How Do Throughput and Speed Affect Clinical Workflow?
Throughput and speed account for 10% of purchasing decisions, directly impacting patient wait times and daily examination capacity. X-ray systems achieve higher throughput rates with 5-10 minute examination times compared to ultrasound requiring 20-45 minutes per study, depending on anatomical complexity. Digital X-ray technology eliminates film processing delays, enabling immediate image review and patient discharge.
Ultrasound workflow depends heavily on operator skill and examination indication, with focused studies completed in 10-15 minutes while comprehensive abdominal evaluations require 30-45 minutes. Facilities should establish protocols for regular maintenance of radiography equipment to prevent downtime that disrupts scheduling and reduces daily capacity.
What Role Does Image Accuracy Play in Modality Selection?
Performance and accuracy represent 24% of purchasing decisions, reflecting the fundamental requirement that diagnostic imaging provide reliable clinical information. X-ray systems deliver consistent image quality with minimal operator dependency, ensuring reproducible results across different technologists and shifts. Detector resolution, dynamic range, and signal-to-noise ratio determine diagnostic confidence for subtle findings like nondisplaced fractures and early pneumonia.
Ultrasound image quality varies significantly based on operator experience, patient body habitus, and equipment capabilities. Advanced beamforming algorithms and harmonic imaging modes improve tissue differentiation and reduce artifacts, but cannot compensate for inadequate operator training.
How Important Is Total Cost of Ownership Compared to Initial Price?
Cost factors constitute 28% of purchasing decisions, while return on investment weighs 16%, and maintenance requirements account for 18% of decision-making priorities. This distribution demonstrates that healthcare administrators recognize that equipment value extends beyond sticker price to encompass operational lifespan and revenue generation potential. Facilities must project patient volume, reimbursement rates, and competitive positioning to calculate break-even timelines for equipment investments.
Initial purchase price represents only 40-50% of the total cost of ownership over 7-10 year equipment lifecycles. Service contracts, supply costs, and upgrade expenses accumulate substantially, making vendor stability and parts availability critical long-term considerations.
Ultrasound Vs. X-Ray Machines: Strategic Considerations for Your Imaging Investment
Successful equipment selection requires aligning technical capabilities with specific clinical applications, patient demographics, and financial constraints. Ultrasound machines provide radiation-free imaging with lower acquisition costs but demand skilled operators and serve limited anatomical applications. X-ray systems deliver rapid skeletal assessment with consistent image quality but require substantial infrastructure investment and expose patients to ionizing radiation.
Facilities should evaluate patient population characteristics, referral patterns, and competitive positioning before committing to major equipment purchases. Geographic location influences access disparities, with rural facilities benefiting from portable ultrasound while urban centers require high-throughput X-ray capabilities. Total cost of ownership analysis must account for maintenance requirements, supply expenses, and potential revenue generation over the equipment’s operational lifespan.
For over four decades, Spectrum Medical X-Ray Company has guided healthcare facilities through complex equipment decisions with transparent pricing and comprehensive lifecycle support. Strategic imaging investments position facilities to deliver superior patient care while maintaining operational efficiency and financial sustainability.
Ready to Find the Right Imaging Equipment for Your Facility?
Choosing between ultrasound and X-ray machines is one of the most important investments your facility will make. At Spectrum Medical Imaging Co., we’ve helped hospitals, imaging centers, private practices, and specialty clinics make confident equipment decisions for over 30 years — backed by transparent pricing, manufacturer relationships, and end-to-end lifecycle support.
Whether you’re upgrading existing equipment, expanding your imaging capabilities, or building a department from the ground up, our team is here to guide you every step of the way. Contact Spectrum Medical Imaging Co. today and let’s find the imaging solution that fits your clinical needs and your budget.
Pricing Disclaimer:
The pricing information displayed on this article is intended for informational purposes only and is subject to change without notice. Actual costs may vary depending on product specifications, quantities, and other factors. For precise pricing and a customized quotation, please contact Spectrum Xray through our web forms.